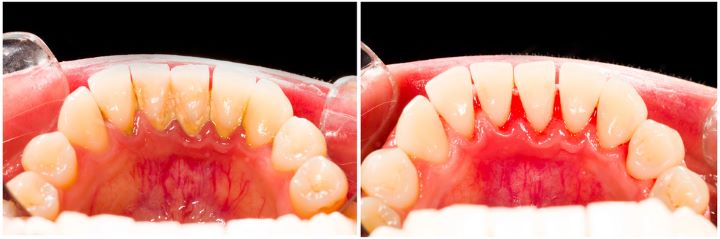
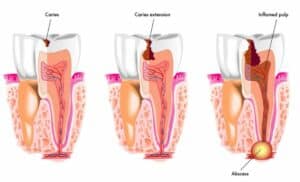
Healthy gums are pink and firm. They should not bleed during cleaning.

However, if bacteria are not cleaned away from the teeth regularly, the surrounding gums can become inflamed. This is called gingivitis. Inflamed gums appear to be large and red in color and can bleed more easily than healthy gums.
Gingivitis is a milder form of gum disease and is reversible. Thorough brushing and flossing can remove the plaque and tartar adhering to the tooth surface while optimizing the oral health of an individual. Also, the bi-yearly scaling and polishing treatment can help reverse inflammation and restore gingival health to normal.
Introduction to Gingivitis
Our mouth is a habitat for millions of microorganisms. Out of all of them, the very famous Streptococcus mutant lives here, too. Though it is a little bacteria, it’s one of the contributors to gingivitis and periodontitis.
Strep and its friends live in your mouth and feed on the sugar and proteins in your food. Once they’re done feeding, they secrete a slimy substance all over your teeth called biofilm.
A little biofilm won’t cause any harm to you. It will harm you if you stop brushing your teeth and the gum tissues twice daily. The biofilm hardens to form plaque and tartar around the teeth. Nearly half of Americans don’t brush their teeth enough.
And when the food builds up on your teeth, you’re inviting Strep and its friends to an opportunistic party. They are destructive, causing your gums to irritate, leading to tenderness and bleeding. Ultimately, this leads to a mild form of gum disease called gingivitis.
It’s just the start…
Guess What Happens Next? The Periodontitis
Ouch! You’re at the risk of developing periodontal disease. Sooner or later, this inflammation of the gums progresses. It triggers your immune system, which sends the fighter cells to fight the naughty bacteria. In an attempt to expel the bacteria, the body’s fighter cell causes further damage to your self-tissues and bone. A few months down the line, the same tissue and the bone will die, leading to a more severe condition called periodontitis.
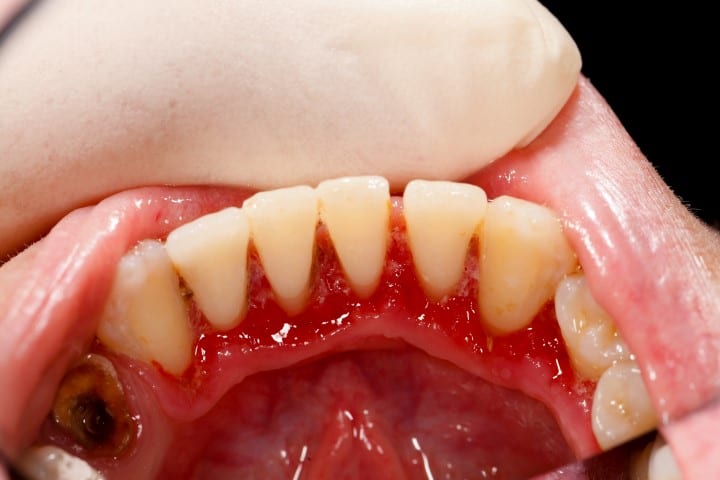
At this point, you will suffer from a periodontal disease, so you have no more structural support. The gums separate from your teeth, forming the periodontal pockets, which can be measured with a periodontal probe. These pockets allow the Strep and its friends to go beneath the gum line. Your bones and gums will no longer support your teeth in place, leading to tooth loss.
It’s not just you. According to the American College of Prosthodontics, 178 million Americans have at least one missing tooth, while according to the American Dental Association, 1 in 3 adults 65 years or older have lost six or more teeth.
Here’s The Caveat
Strep and its friends can enter your bloodstream through your gums. These naughty bacteria can affect your kidneys, leading to chronic kidney disease. People with periodontal disease are 4x more prone to chronic kidney disease than people with healthy gums.
Causes of Gingivitis
- Poor oral hygiene is a common cause of gingivitis. You may suffer from plaque-induced gingivitis when you don’t clean your teeth properly twice a day or skip using an anti-bacterial mouthwash. Or if you have never been for scaling and root planning sessions all your life, you’re still at risk.
- You don’t get a regular dental checkup. Sometimes, gingivitis may trick us. Gingivitis without any symptoms is common in smokers. It might not show up with the typical symptoms like swollen gums, tenderness, and bad breath. It won’t be revealed until it progresses to periodontitis. It’s better to get your regular dental checkup and professional cleaning so your dentist might catch the hidden disease.
- Have crooked or malaligned teeth. Brushing and flossing get difficult in such a scenario. Professional dental cleaning to remove plaque is advisable every six months.
- Uncontrolled diabetes can put you at risk of gingivitis. It causes the blood vessels to thicken, reducing blood flow to the gums.
- Habitual smokers and tobacco chewers are prone to gingivitis. They’re at risk of developing severe gum diseases. The immunosuppressant activity in smokers contributes majorly to gingivitis. Gingivitis can progress to periodontitis in a matter of days in such individuals.
- Drugs contributing to dry mouth or xerostomia can lead to gingivitis. Oral contraceptives, oral glucose-lowering agents, and medications that treat epilepsy are a few contributors.
- Pregnancy can lead to hormonal changes, ultimately affecting the overall health of the teeth and gums. To prevent gingivitis or reverse gingivitis in pregnancy, one must take better care of oral health.
Signs and Symptoms of Gingivitis

- Bleeding gums: The inflamed gums appear to be red in color. They appear to be swollen. The process of inflammation increases the amount of blood vessels at the infected site causing the gums to bleed on eating and brushing.
- Bad breath or a metallic taste: A persistent bad breath or metallic taste in your mouth signifies gum disease. The plaque is a thin film made up of food buildup and bacteria. The bacteria altogether produces toxins which gives fetid odor and metallic taste whenever they feed on the food accumulates.
- Tooth sensitivity or pain on chewing: When the gums recede, the tooth root surfaces get exposed. This directly triggers the nerves of the tooth leading to tenderness and sensitivity.
- Gum recession: With the receded gums, the roots of your teeth get exposed. This makes your teeth longer than normal.
Types of Gingivitis
There are two major types of gingivitis:
- Plaque-induced Gingivitis
- Non-Plaque Induced Gingivitis
The plaque-induced gingivitis is caused by inadequate oral hygiene or proper home care.
The non-plaque-induced gingivitis can be caused by viral, systemic, local exposure to chemicals, and more.
Role of Dentist in Treating Gingivitis
If you think you’ve the above-stated symptoms see your dentist. He will take your detailed history before performing an intra and extra-oral examination.
Firstly, he’ll ask you a few questions to know your symptoms of gum disease.
Your dentist will assess your oral hygiene and look for plaque, calculus, and tartar on your tooth surface. He will also look for probing depths with a periodontal probe around the tooth.
He might get some dental radiographs to assess the bone health and the health of the periodontal tissues that secure your tooth.
Later, he’ll brief you about different types of gum diseases before providing you with the treatment options.
Treatment of Gingivitis

Gingivitis is reversible and is curable. It can be done in two ways:
Revamping Your Oral Hygiene At Home Routine:
- Brush twice daily.
- Brushing with a proper brushing technique.
- Floss once daily.
- Use antibacterial mouthwash.
- Rinse your mouth with water after every meal.
Two to three weeks of oral hygiene at home can reverse all the signs and symptoms of gum disease you face today.
Professional Dental Cleaning
Scaling and root planing are the keys to removing plaque, tartar, and calculus from above and below the gum line. Visit your dentist or dental hygienist to eliminate the symptoms associated with gingivitis. Untreated gingivitis can lead to periodontitis, so you must carefully plan your dental visits.
Reverse Your Gingivitis In Two Weeks With These Super Effective Techniques
Water Flosser:
Water flossers are not an alternative to traditional string flossers; these do wonders. Gingivitis is an inflammation, and when you’re trying to reverse it, stimulation from a water flosser can help reduce the soreness of your gums.
Warm Salt Water Rinses
Warm salt water rinses provide a soothing effect to your inflamed gums. This creates an alkaline environment in your mouth where bacteria can no longer thrive.
FAQs
What is the proper brushing technique for gingivitis?
According to the American Dental Association, manual and electronic toothbrushes are equally effective in removing plaque. However, manual toothbrushes are often not used correctly to reverse the mild symptoms associated with gingivitis. A brushing technique named Stillman’s Technique is popular for reversing gingivitis.
Place the toothbrush at a 45-degree angle towards the gum line. Vibrate the brush back and forth 15 to 20 times while maintaining the angulation. Move the brush towards the chewing surface of the teeth to remove the food debris from the gingiva. Repeat this step for all the surfaces of the teeth until you’re done cleaning your whole mouth.
How does smoking cause gingivitis?
According to the CDC, if you’re a smoker, you’re at twice the risk of developing gum disease than a non-smoker. Smoking reduces your immunity, making it difficult for your body to fight the gum infection. And once the damage occurs, the healing gets delayed and deranged in the smokers.